Wellfleet Student plans are designed with the goal of member satisfaction, by delivering the right care, at the right place, for the right price. Through a partnership with Cigna, Wellfleet provides its student members access to more than 1,000,000 providers at more than 6,000 facilities nationwide. In addition to having a great network partner, we have a passionate internal team that works tirelessly for our members. This includes customer service, a quality assurance department, and provider and clinical team, with oversight from our Chief Medical Officer.
Wellfleet’s Provider Network team
Our Provider Network team works closely with network partners and vendors to ensure our members have access to high quality, in- and out-of-network care. As faithful stewards to our members, the team works with providers on a case-by-case basis, to help reduce their out-of-pocket responsibility and retain cost for the health plan.
Not satisfied with business as usual
When high-dollar claims come into Wellfleet, there are several internal teams that review them. This is to ensure the bill is appropriate for the care provided. The steps in their process ensures proper evaluation, to provide the fairest outcome for the member and the plan. Most times these high-dollar claims are appropriate, and the approval is seen as business as usual. However, some raise flags based on things like billing, coding, or prior treatments.
Unrelated charges uncovered
A student member’s 10-month-old needed a minor procedure to correct a cleft pallet. The need for the repair was simple. The repair would help with the child’s speech later in life. This is because a child with an unrepaired cleft palate cannot stop air from rushing out of their nose during speech. This makes it very difficult for them to learn how to speak correctly and difficult for others to understand what they are saying.
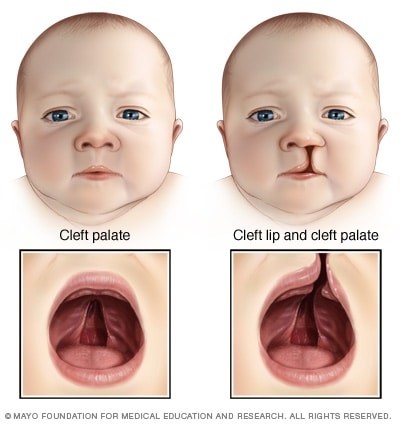
The member was able to schedule an in-network procedure with their preferred provider and the procedure was a success. Post-surgery, the child stayed at the hospital for one day, (typical for this procedure) and returned home the following day without issue.
When the billing came in for the procedure, the examiner was surprised to see that there were additional charges that were unrelated to the principal diagnosis. Upon further research, the payment integrity team found that none of the additional procedures were conducted. So, they contacted the provider to correct the error.
This finding helped save the member almost $2,000 in out-of-pocket fees and saved the plan almost $20,000!
Learn more about Wellfleet Student’s commitment to our clients and member.


