Wellfleet Student plans are designed with the goal of member satisfaction, by delivering the right care, at the right place, for the right price. Through a partnership with Cigna, Wellfleet provides its student members access to more than 1 million providers at more than 6,000 facilities nationwide. In addition to having a great network partner, we have a passionate internal team that works tirelessly for our members. This includes customer service, a quality assurance department, and provider and clinical team, with oversight from our Chief Medical Officer.
Wellfleet’s Payment Integrity team
Our Payment Integrity Team works closely with network partners and vendors to ensure our members have access to high quality, in- and out-of-network care. As faithful stewards to our members, the team works with providers on a case-by-case basis, to help reduce their out-of-pocket responsibility and retain cost for the health plan.
Not satisfied with business as usual
When high-dollar claims come into Wellfleet, there are several internal teams that review them. This is to ensure the bill is appropriate for the care provided. The steps in their process ensures proper evaluation, to provide the fairest outcome for the member and the plan. Most times these high-dollar claims are appropriate, and the approval is seen as business as usual. However, some raise flags based on things like billing, coding, or prior treatments.
Providing coverage for student’s unexpected needs
Wellfleet Student plans are designed to ensure that student members have coverage for the routine, as well as the unexpected. Like when one member visited their primary care doctor due to recurring episodes of headaches and vertigo.
The student member had no previous history of headaches or vertigo, so scheduled a checkup to discuss with their primary care doctor. After a routine examination, their doctor recommended a CT scan to help with a diagnosis. The CT scan uncovered the culprit – a cerebellar cystic lesion. This is a sac filled with air, fluid or other material, located on the portion of the brain on the back of the head between the cerebrum and brain stem1; see image below.
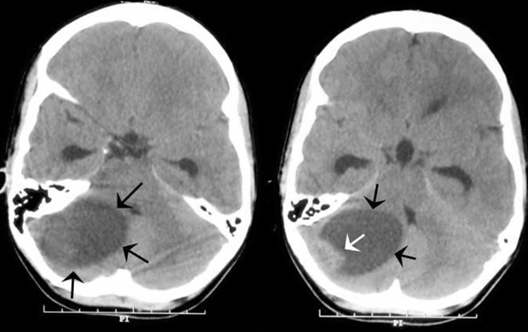
Source: Researchgate.net
Once discovered, the medical team consulted with the student on next steps, and surgery was scheduled to remove the lesion at a local hospital. We’re happy to report the procedure was a success with no complications, and the member was discharged four days after the surgery.
Payment integrity review – coding shows major complications
Upon reviewing the initial billing from the hospital, the payment integrity team noted coding that showed major complications during the procedure. From a deeper review of the medical records and doctor notes, they determined that this did not align with what had occurred, and followed up with the provider. In their discussions, the provider agreed on the oversight and updated the billing to reflect the correct coding for the procedure.
This review and update led to the overall savings to the plan being reduced by more than $35,000. Further, this saved the member $3,500 in out-of-pocket expenses!
Don’t miss another great savings story! Sign up for our monthly clinical newsletter and get member savings stories in your inbox with other great Wellfleet Student happenings.
Resource
1 Mayo Clinic. (n.d.) Tumor vs. Cyst: What’s the difference. Retrieved on September 12, 2022, from https://www.mayoclinic.org/diseases-conditions/cancer/expert-answers/tumor/faq-20057829


